Not every IVF cycle uses the same fertilization method, and that difference matters more than most people realize. Intracytoplasmic sperm injection, or ICSI, is a specialized technique used within IVF that involves injecting a single sperm directly into an egg. While it has helped many couples overcome severe male infertility, it is not the right choice for every patient. Understanding when ICSI is genuinely beneficial, when it offers no added advantage, and what risks it carries can help you ask better questions and make more informed decisions about your fertility care.
Table of Contents
- What is ICSI and how does it work in IVF?
- How ICSI compares to standard IVF: Success rates and limitations
- Risks and controversies: The safety of ICSI for families
- Who should consider ICSI? Patient selection and expert guidance
- A balanced approach: Why ‘more technology’ isn’t always better
- Take the next step: Advanced fertility expertise in Southern California
- Frequently asked questions
Key Takeaways
| Point | Details |
|---|---|
| ICSI explained | ICSI is a method where a single sperm is injected directly into an egg, used within certain IVF cycles. |
| Not for everyone | ICSI is most beneficial for severe male infertility or previous fertilization issues, not all IVF patients. |
| Success and safety | Success rates for ICSI and standard IVF are similar in many cases, and risks are low for both methods. |
| Personalized care matters | Choosing ICSI should be based on your unique fertility profile and a discussion with your specialist. |
What is ICSI and how does it work in IVF?
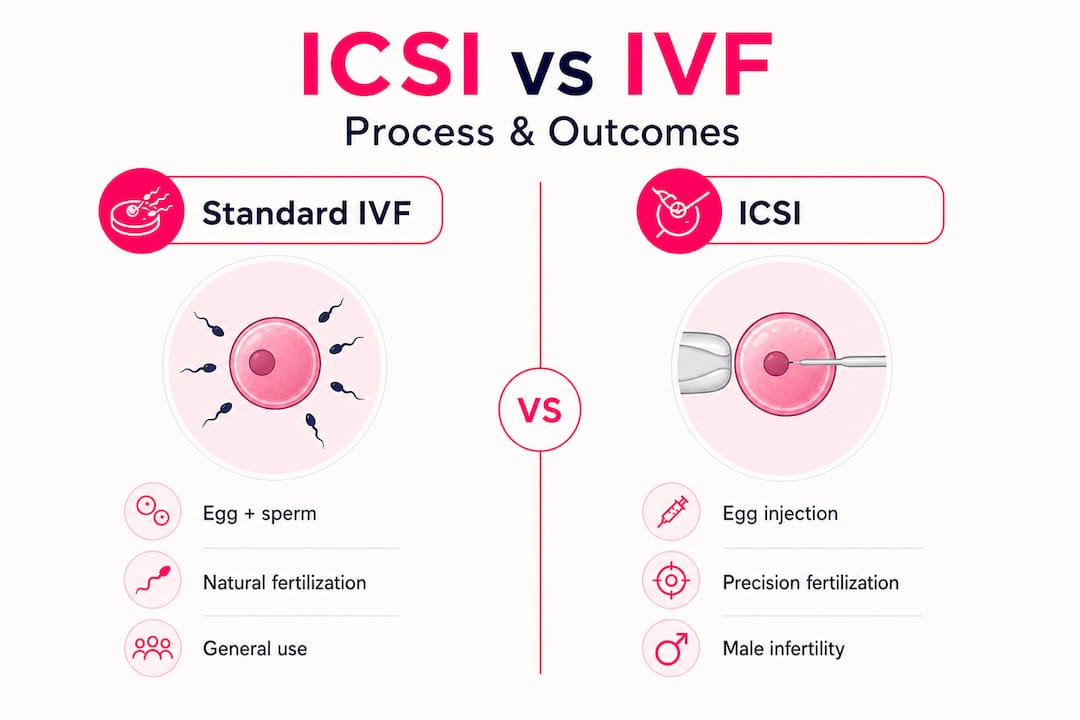
In a standard IVF cycle, retrieved eggs are placed in a dish alongside thousands of sperm and fertilization happens naturally when one sperm penetrates the egg on its own. ICSI changes that process entirely. With ICSI, an embryologist selects a single sperm under a high-powered microscope and injects it directly into the center of a mature egg using a fine glass needle.
The rest of the IVF cycle remains the same. Eggs are still retrieved after ovarian stimulation, embryos are still cultured in the lab, and the best-quality embryo is transferred to the uterus. The only difference is how fertilization occurs.
ICSI was originally developed in the early 1990s to address severe male infertility cases where sperm could not penetrate the egg on their own. Before ICSI, men with very low sperm counts or poor sperm motility had almost no path to biological parenthood through IVF. The procedure changed that reality significantly.

Today, ICSI is used in a wide range of clinical scenarios, not just severe male infertility. Reviewing your fertility treatment options with a specialist helps clarify whether ICSI is appropriate for your specific situation. Patients considering lower-stimulation protocols should also understand how ICSI fits within a Mini IVF approach, since fewer eggs retrieved can make precise fertilization even more critical.
When ICSI is typically considered:
- Severe oligospermia (very low sperm count)
- Asthenospermia (poor sperm motility)
- Teratospermia (abnormal sperm morphology)
- Obstructive or non-obstructive azoospermia (no sperm in ejaculate, requiring surgical retrieval)
- Previous IVF cycles with poor or failed fertilization
- Use of frozen eggs, where the zona pellucida (outer shell) can harden
- High sperm DNA fragmentation
Research shows that fresh testicular sperm may rescue ICSI failure in non-obstructive azoospermia over cryopreserved sperm, and that high sperm DNA fragmentation benefits from using testicular rather than ejaculated sperm. These are nuanced clinical decisions that require specialist input.
| Feature | Standard IVF | ICSI |
|---|---|---|
| Fertilization method | Natural (sperm + egg in dish) | Direct sperm injection into egg |
| Sperm required | Thousands | One viable sperm |
| Best for | Normal sperm parameters | Male factor infertility, prior IVF failure |
| Lab complexity | Lower | Higher (requires micromanipulation) |
| Additional cost | Included in base IVF | Usually an add-on fee |
Pro Tip: ICSI is not a default upgrade for all IVF cycles. Many clinics use it broadly, but evidence supports selective use based on specific clinical indications. Ask your specialist whether ICSI is recommended for a medical reason in your case, not just as a precaution.
The Precision IVF approach at Life IVF Center is built around exactly this kind of individualized thinking. Rather than applying the same protocol to every patient, the team evaluates each person’s unique biology before recommending whether ICSI belongs in the treatment plan. You can also review IVF basics to build a foundation before your consultation.
How ICSI compares to standard IVF: Success rates and limitations
With a clear picture of the ICSI process, let’s see how it measures up against standard IVF when it comes to results.
The evidence on ICSI versus conventional IVF is more nuanced than many people expect. For couples dealing with severe male infertility, ICSI clearly improves fertilization rates and gives sperm that could never penetrate an egg on their own a real chance. But for couples without a diagnosed sperm problem, the story is different.
In non-severe male factor cases, randomized controlled trials show no significant improvement in cumulative live birth rates with ICSI versus standard IVF, with figures like 43.2% for ICSI compared to 47.3% for conventional IVF. That data challenges the assumption that ICSI always produces better outcomes.
Situations where ICSI shows clear benefit:
- Severe male factor infertility with very low counts or motility
- Zero sperm in ejaculate requiring surgical sperm retrieval
- Repeated fertilization failure in prior IVF cycles
- Frozen egg thaw cycles where zona hardening can block sperm entry
- Preimplantation genetic testing (PGT) cycles, where reliable fertilization is critical
Situations where ICSI may not improve outcomes:
- Mild or moderate male factor infertility
- Unexplained infertility with normal sperm parameters
- Couples with no prior fertilization failure
- Older female patients where egg quality, not fertilization, drives outcomes
Key finding: A large randomized controlled trial found that routine ICSI use in couples without severe male factor infertility did not produce higher live birth rates than conventional IVF. This suggests that using ICSI broadly, without clinical justification, adds cost and procedural complexity without improving results.
If you have questions specifically about sperm health, reviewing common male fertility questions can help you understand what test results mean and how they influence treatment decisions.
The takeaway is not that ICSI is overrated. It is that ICSI is a precision tool. Used in the right clinical setting, it is highly effective. Applied indiscriminately, it adds expense and lab manipulation without a meaningful benefit to the patient.
Risks and controversies: The safety of ICSI for families
But as with any medical procedure, it’s important to look honestly at the possible downsides of ICSI.
Most people who go through ICSI have healthy babies. The absolute risks are low. But being fully informed means understanding what those risks are, how they compare to standard IVF, and what current research says about their causes.
Risks of ICSI include potential egg damage during the injection process, a slightly elevated rate of certain congenital anomalies such as hypospadias (a urethral opening abnormality in boys) and imprinting disorders like Angelman syndrome. Importantly, researchers continue to debate whether these risks stem from the ICSI procedure itself or from the underlying infertility that makes ICSI necessary in the first place.
That distinction matters. Many of the genetic and developmental factors that contribute to male infertility may also independently increase the risk of certain conditions in offspring. Separating the effect of the procedure from the effect of the underlying condition is methodologically difficult, and most studies have not been able to do so definitively.
Known risks associated with ICSI and how clinics minimize them:
- Egg damage during injection: Skilled embryologists and high-quality micromanipulation equipment significantly reduce this risk. Damage rates at experienced centers are typically low.
- Slightly elevated congenital anomaly rates: The absolute increase is small. Genetic counseling before treatment can help families understand their personal risk profile.
- Transmission of male infertility to male offspring: If the cause of male infertility is genetic (such as Y chromosome microdeletions), sons conceived via ICSI may inherit the same condition. Preimplantation genetic testing can screen for some of these issues.
- Imprinting disorder risk: Research suggests a marginally elevated risk of rare imprinting disorders, though these conditions remain uncommon overall.
“The absolute risk of birth defects with ICSI remains low, and much of the observed increase may reflect the genetic background of infertile men rather than the procedure itself.” This is why a thorough evaluation of both partners before treatment is so important.
Understanding what to expect throughout your IVF journey, including how ICSI fits into the overall process, is easier when you have a clear IVF experience overview to reference. Transparency about both the benefits and limitations of each procedure is central to how Life IVF Center approaches patient care.
Who should consider ICSI? Patient selection and expert guidance
So how do you know if ICSI should be part of your treatment plan? Let’s break down when the experts recommend it.
Patient selection is where clinical expertise makes the biggest difference. ICSI is not a blanket solution, and the decision should be based on a thorough workup of both partners, including semen analysis, sperm DNA fragmentation testing when indicated, and a review of any prior fertility treatment history.
Clinical scenarios where ICSI is clearly recommended:
- Severe oligospermia or azoospermia: When sperm counts are extremely low or absent from ejaculate, ICSI with surgically retrieved sperm is often the only viable path to fertilization.
- Repeated fertilization failure: If a previous IVF cycle produced eggs but few or no fertilized embryos, ICSI in the next cycle can address the problem directly.
- High sperm DNA fragmentation: When fragmentation levels are elevated, fresh testicular sperm used with ICSI tends to produce better outcomes than ejaculated sperm, as testicular sperm has lower fragmentation.
- Frozen egg cycles: Eggs that have been vitrified and thawed have a harder zona pellucida, making natural sperm penetration less reliable. ICSI improves fertilization rates in these cycles.
- Preimplantation genetic testing cycles: Reliable fertilization is essential when embryos will be biopsied for genetic screening, making ICSI the preferred method.
- Use of surgically retrieved sperm: Whether from obstructive or non-obstructive azoospermia, sperm retrieved directly from the testis or epididymis requires ICSI for fertilization.
- Very low egg yield: When only a small number of eggs are retrieved, ICSI maximizes the chance that each egg will fertilize successfully.
Nuanced situations also exist. For couples using donor sperm with normal parameters, ICSI may not add benefit. For same-sex female couples or single women using donor sperm, the decision depends on sperm quality and egg response. Understanding third-party reproduction options can clarify how ICSI fits into those pathways.
Pro Tip: Before agreeing to ICSI, ask your specialist to explain the specific clinical reason it is being recommended for your case. If the answer is “just to be safe” without a documented indication, that is worth discussing further. Evidence-based patient selection leads to better outcomes and avoids unnecessary cost.
Reviewing your insurance for IVF coverage is also worthwhile, since ICSI is often billed as a separate add-on and may or may not be covered depending on your plan and state mandates.
A balanced approach: Why ‘more technology’ isn’t always better
There is a tendency in fertility medicine, as in many areas of healthcare, to equate more intervention with better care. ICSI is a powerful example of why that assumption deserves scrutiny.
When ICSI was first introduced, it was rightly celebrated as a breakthrough for men with severe infertility. Over the following decades, its use expanded far beyond that original population. Today, ICSI is used in the majority of IVF cycles in many countries, including a large proportion of cases where there is no documented male factor infertility. The data, however, does not support that broad application.
This is not a criticism of ICSI as a technology. It is a call for precision. The same clinical rigor that makes ICSI effective for the right patient makes it unnecessary and potentially counterproductive for the wrong one. Adding micromanipulation to every cycle introduces procedural variables, increases cost, and does not improve outcomes in patients who would fertilize normally with conventional IVF.
At Life IVF Center, the philosophy behind personalized IVF strategies is grounded in this thinking. Every treatment decision, including whether to use ICSI, should be driven by the individual patient’s biology, history, and goals. Not by habit, not by convenience, and not by the assumption that newer or more complex always means better.
The couples who benefit most from fertility care are those whose treatment is matched carefully to their actual needs. That requires honest conversations, thorough testing, and a willingness to recommend a simpler approach when the evidence supports it. Precision medicine in fertility is not about using every available tool. It is about using the right tool for the right patient at the right time.
Take the next step: Advanced fertility expertise in Southern California
With this information in mind, you might be ready to explore your own fertility journey with expert support.
Life IVF Center offers individualized consultations designed to determine whether ICSI, standard IVF, or another approach is the right fit for your situation. The team reviews your complete diagnostic picture before making any protocol recommendations, so you never receive a one-size-fits-all plan.
Whether you are just beginning to research IVF treatment options or you have already been through a cycle and want a second opinion, the specialists at Life IVF Center are equipped to guide you. Explore Precision IVF options to understand how customized protocols are built around your biology. If male infertility is part of your picture, dedicated male fertility services are available to ensure sperm health is thoroughly evaluated before any treatment decision is made. Serving patients across Southern California, Life IVF Center combines advanced science with genuinely personalized care.
Frequently asked questions
Does ICSI increase the chance of twins or multiples compared to regular IVF?
ICSI itself does not increase the chance of twins. The number of embryos transferred, not the fertilization method, determines the likelihood of a multiple pregnancy.
Is ICSI recommended for all couples with unexplained infertility?
No. Randomized controlled trials show no significant improvement in cumulative live birth rates with ICSI versus standard IVF in non-severe male factor cases, making routine use in unexplained infertility unsupported by current evidence.
Does ICSI put my baby at higher risk for birth defects?
ICSI is associated with a slightly elevated risk of certain birth defects, but the absolute increase is small and may reflect the underlying infertility rather than the procedure itself.
Are there cases where ICSI is essential?
Yes. ICSI is essential for severe male infertility, cases where testicular sperm must be used, and situations involving repeated fertilization failure or frozen egg cycles where natural sperm penetration is unreliable.
Does ICSI cost more than standard IVF?
Yes, ICSI typically adds an additional fee to the base cost of an IVF cycle because it requires specialized lab equipment and highly trained embryologists to perform the micromanipulation procedure.
Recommended
- Fertility treatment options: Effectiveness and best uses
- Intrauterine Insemination (IUI) – Life IVF Center
- Mini IVF: A personalized path to fertility success
- Egg retrieval tips: Expert guidance for IVF success